Embryo reduction is the practice of reducing the number of foetuses in a multifetal pregnancy (those involving more than one foetus) to a twin or singleton pregnancy, without targeting a specific foetus for reduction… This procedure is often performed after a congenital defect has been identified. The aim of multifetal reduction is to avoid the medical issues generally related to multiple births (including premature births, low birth weights and associated medical problems).
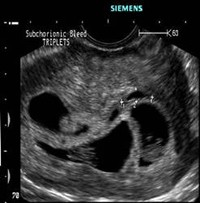
PROCEDURE
The reduction procedure is generally carried out during the first trimester. The most common method is to inject a chemical solution or feticide into the foetus or fetuses selected for either genetic reasons or for ease of accessibility. At our clinic we inject potassium chloride into or in the vicinity of the foetal heart thereby causing it to stop functioning under general anaesthesia under sonography guidance by embryo reduction needle introduced transvaginally. Generally, the fetal material is reabsorbed into the woman’s body. Patient is treated like a case of threatened abortion.
Reduction does have its own risks, including the possibility that one or more of the remaining fetuses will also die or complete abortion of all the foetuses but this risk is much less as compared to the risk of abortion and premature labour associated with multiple pregnancies along with their attendant problems.
